Think of the camera on your smartphone for a moment. You know that, generally, more megapixels mean a sharper photo where you can zoom in tight and still see fine textures, like the weave of a shirt or individual strands of hair. Medical imaging works on a very similar principle, but the stakes are obviously much higher than a blurry vacation photo. We call this critical factor spatial resolution radiology. It essentially dictates whether an image looks crisp or blurry, which directly impacts a doctor’s ability to spot tiny, life-threatening abnormalities.
High spatial resolution allows radiologists to:
- Distinguish between two tiny, adjacent structures without them blurring into a single blob.
- Visualize sharp edges on subtle, hairline bone fractures.
- Detect minute micro-calcifications in breast tissue that signal early cancer.
Without this clarity, distinct pathologies merge into indistinguishable shadows, potentially hiding the early warning signs of disease.
Defining the Concept in the Real World
At its core, spatial resolution radiology defines an imaging system’s ability to differentiate between two objects that are sitting very close to one another. Imagine you are looking at two small pebbles on the ground from a mile away; to your eye, they likely look like one big rock. As you walk closer, effectively improving your resolution, you eventually see they are distinct entities. In a hospital setting, this capability is the difference between seeing a clear, defined break in a small wrist bone and just seeing a vague, gray shadow.
Radiologists heavily rely on this sharpness to make decisions. If a system suffers from poor resolution, a small tumor might blur into the surrounding healthy tissue, effectively making it invisible to the human eye. Therefore, achieving high spatial resolution radiology isn’t just a technical benchmark for physicists; it is a clinical necessity for accurate diagnosis and timely treatment.
Why We Chase the Details
You might wonder, why do we need such extreme detail for every single scan? The answer lies in the pathology itself. Many diseases start small.
- Breast Cancer: Often manifests initially as tiny specks of calcium called micro-calcifications. These can be smaller than a grain of sand. To see these, mammography requires the highest spatial resolution radiology of any standard imaging modality. If the image is even slightly blurry, those specks disappear, and the cancer goes undetected until it grows larger.
- Lung Disease: The interstitium of the lung is a delicate, lace-like web of tissue. When diseases like pulmonary fibrosis attack, they thicken this web in very subtle ways. A high-resolution CT scan captures these fine reticular patterns, whereas a standard scan might just show general “haziness.” Consequently, doctors specifically order “High-Resolution CT” (HRCT) when they need that boosted spatial resolution radiology to actually see the texture of the lung tissue.
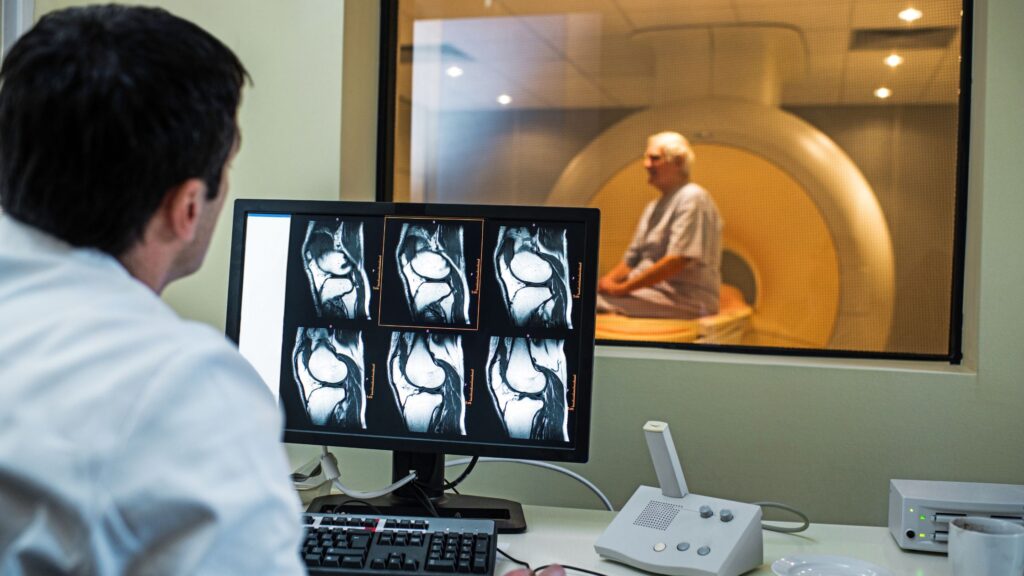
How Different Modalities Handle Resolution
Different machines operate under different physical laws, so they have different limitations. It is definitely not a “one size fits all” situation.
1. X-Ray and Mammography In basic X-ray, the geometry matters immensely. The source of the X-ray beam, known as the focal spot, acts somewhat like the sun casting a shadow.
- A large focal spot creates a fuzzy edge (penumbra).
- A small focal spot creates a sharp, defined edge.
Technologists often consciously select a smaller focal spot to improve spatial resolution radiology when looking for fine detail. However, the digital detector also plays a massive role here. You simply cannot resolve a detail smaller than the physical pixel on the detector plate.
2. Computed Tomography (CT) CT scanners are inherently more complex. Here, resolution largely depends on the pixel size and slice thickness.
- Pixel Size: You calculate this by dividing the Field of View (FOV) by the Matrix size. If you focus the scanner on a small area (small FOV) but keep the grid of pixels the same (large matrix), your pixels effectively get smaller. Smaller pixels mean significantly better spatial resolution radiology.
- Slice Thickness: Thick slices cause “partial volume averaging,” where different tissues are mashed together in the vertical direction. Thin slices solve this problem, keeping the data crisp.
3. Magnetic Resonance Imaging (MRI) MRI is a beast of its own. It uses 3D pixels called voxels. To improve detail, we need smaller voxels. We achieve this by using stronger magnetic gradients and altering the way we sample data. But MRI faces a unique hurdle: time. Increasing the spatial resolution radiology usually requires much longer scan times. If the scan takes too long, the patient might twitch, cough, or breathe heavily, blurring the image and ruining the resolution anyway.
4. Ultrasound Sound waves behave differently than ionizing radiation. In ultrasound, resolution actually changes depending on where you look. Axial resolution depends on frequency. High-frequency probes (like 12-15 MHz) give amazing detail for superficial structures but cannot penetrate deep into the abdomen. So, sonographers constantly swap probes to balance the need for depth with the need for spatial resolution radiology.
The Inevitable Trade-offs: The “No Free Lunch” Rule
This is perhaps the most important concept to grasp: you cannot simply turn a dial and get perfect resolution without paying a price. Medical physics is a game of constant trade-offs.
- The Noise Penalty: When you make pixels smaller to get better detail, each pixel catches fewer photons (in X-ray/CT) or less signal (in MRI). This drops the Signal-to-Noise Ratio (SNR). The image becomes grainy, much like a photo taken in a dark room. To fix this graininess while keeping high spatial resolution radiology , you have to increase the radiation dose. This brings up ethical safety concerns regarding patient exposure.
- The Time Penalty: As we touched on with MRI, high detail takes time. A high-resolution brain scan might take 45 minutes, while a standard one takes 20. In a busy emergency room where every second counts, doctors might accept lower spatial resolution radiology just to get an answer quickly to save a life.
- The Patient Factor: We often forget that patients are human beings, not mannequins. They breathe, their hearts beat, and they have tremors. Even the world’s most advanced scanner cannot fix motion blur. If a patient moves just a few millimeters, the effective resolution drops instantly. Therefore, comforting the patient and restraining motion is just as important as the engineering behind spatial resolution radiology.
Measuring the Sharpness
How do we actually know if a machine is performing well? Physicists use specific tools to measure this.
- Line Pairs per Millimeter (lp/mm): This is the most common metric. Physicists use a test object with lead lines that get closer and closer together. They look at the image to see at what point the black and white lines turn into a gray smear.
- Mammography: ~15-20 lp/mm (Extreme detail).
- General X-Ray: ~3-5 lp/mm.
- CT: ~0.7 lp/mm.
- Modulation Transfer Function (MTF): This is an advanced metric. It is a complex graph that tells us how well the system preserves contrast as details get smaller. It is the gold standard for characterizing spatial resolution radiology in a lab setting, ensuring that the equipment meets the rigorous standards required for patient care.
When Radiology Meets Art
- We usually think of X-rays as purely medical—stark, black-and-white, and usually bad news. But have you ever seen Skiagraphy? It’s a niche style where photographers ditch the standard camera lens for an X-ray tube.
- The vibe is totally different. They aren’t capturing the surface of a rose; they’re revealing the ghost inside it—the delicate veins and hidden structures we normally ignore. It’s weirdly beautiful to see a harsh diagnostic tool used to create such soft, intricate art. It just goes to show that even in a field as technical as radiology, there’s plenty of room for creativity.
Conclusion
Mastering the nuances of image quality is a lifelong pursuit for imaging professionals, but the basics remain clear. Spatial resolution radiology is the technical parameter that directly translates into the clinical ability to see the fine details that matter most. It is the difference between uncertainty and a confident diagnosis. By balancing physical constraints with clinical needs, medical teams ensure that every image provides the clearest possible window into the human body.
For more insights and daily updates on medical imaging technology, visit Zero Theories.
Disclaimer: This article is intended for informational purposes only and does not constitute medical advice or professional training in radiology. Always consult with a qualified healthcare professional for medical diagnosis and treatment.

Leave a Reflection